Sclerotherapy: What is it? How Does it Work?
 Sclerotherapy is a versatile treatment that targets spider veins, varicose veins, and other vein issues. It has been tried and tested over many years and has proven to be very effective. If you have any of these vein issues, this procedure may be right for you.
Sclerotherapy is a versatile treatment that targets spider veins, varicose veins, and other vein issues. It has been tried and tested over many years and has proven to be very effective. If you have any of these vein issues, this procedure may be right for you.
What is Sclerotherapy?
Sclerotherapy is a minimally-invasive procedure that treats spider and varicose veins. Depending on how deep the abnormal vein is under your skin, your doctor may need to use ultrasound technology to see where the vein is located. Then, he or she will inject a specialized solution directly into the target vein. This solution is usually saline-based, but the chemical agent depends on the size of the vessel that needs to be treated.
Sclerotherapy will not only improve the appearance of veins, but it will improve venous blood flow and lower chronic swelling as well.
How Does Sclerotherapy Work?
Injecting the saline solution into a vein damages the inside lining of the vessel. This forms a clot that blocks circulation in the vein. This forces the body to reroute blood flow through healthier veins. The damaged vein will eventually become scar tissue and the body will reabsorb it under the skin. This absorption causes the vein to fade from view.
Who is a Possible Candidate for Sclerotherapy?
Anyone who is in general good health and experiences unsightly spider or varicose veins is a good candidate for sclerotherapy. It can also be helpful for someone who suffers from venous insufficiency and cannot control the issue with the use of compression stockings.
Causes of Spider or Varicose Veins
There are a number of things that increase a person’s risks of developing vein issues.
Genetics. Almost half of the population of people who develop varicose veins have family members with the problem.
Age. As a person gets older, wear and tear cause vein valves to become weak.
Obesity. When a person is overweight, the extra weight strains the veins.
Gender. Women are much more likely to develop varicose veins. Hormones, pregnancy, and menopause increase the risks of development.
Prolonged Sitting or Standing. When a person sits with his or her legs bent, the veins must work harder to push blood to the heart.
What to Expect During the Procedure
When the procedure is about to begin, the patient lays on his or her back with legs elevated. Your doctor will clean the area and then insert the needle. When he or she removes the needle, the doctor will apply compression and then massage the area to prevent blood from entering the vessel. Immediately the following sclerotherapy, the patient will need to stand and walk so blood clots do not form.
Is Sclerotherapy Painful?
Sclerotherapy does require an injection into the skin, so the patient may experience some stinging or cramps when the syringe is inserted. Also, some feel pain from the saline solution being injected into the vein. The procedure should be otherwise pain-free unless a rare difficulty occurs.
All medical procedures pose a risk, but your doctor will discuss side effects before deciding if this therapy will work for you. For example, a person may experience hyperpigmentation (darkening of the skin), pain at injection site, temporary swelling, or an allergic reaction. In severe cases, a person may experience nerve damage.

Recovery and Aftercare of Sclerotherapy
Sclerotherapy is performed on an outpatient basis; therefore, patients do not require hospitalization. Following the treatment, the patient will need to wear compression dressings for up to three weeks. A follow-up appointment after this recovery time will determine if further action is necessary.
After treatment, veins will fade within a few weeks. On rare occasions, it may take more than a month to see total results. More than one treatment may be necessary for larger veins.
Is Sclerotherapy Covered by Insurance?
Since sclerotherapy is often linked to the correction of spider veins, some see it as purely cosmetic. In these cases, most insurance companies will not cover the elective procedure. However, it can be used for other medical purposes, and if so, a doctor must document a patient’s condition. An insurance provider may cover the procedure if they understand the problems associated with a malfunctioning deep vein.
If you suffer from varicose veins or spider veins, you may wish to consider sclerotherapy. Contact us to ask any additional questions you may have or to schedule a consultation where our providers will meet with you to discuss the issues you are facing and establish a plan of action.
Lear MoreVARICOSE VEINS: DEFINITION, CAUSES AND TREATMENT
Varicose veins and spider veins: We always hear them spoken in the same breath. Are they the same, though? Should you be worried about the affect varicose veins can have on your health? Let’s take a look at the most commonly asked questions regarding varicose veins.
What Are Varicose Veins and How Are They Different from Spider Veins?
Varicose veins are enlarged, twisted veins that are visible at skin level. Varicose veins indicate that blood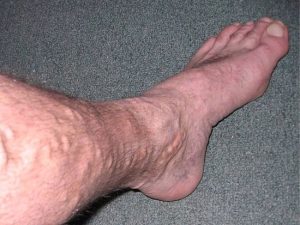 is not flowing smoothly throughout the pathways.
is not flowing smoothly throughout the pathways.
Varicose veins are usually bigger and deeper than spider veins and are typically located in the legs. They are more major blood return pathways, however, there are numerous “collateral” veins that pick up the slack once the varicose vein is eliminated.
This is an important note because a common misconception/fear around treating varicose veins is you are eliminating important pathways for your blood. In reality, this allows the other veins to work better because blood is avoiding a path where there is resistance.
Instead, blood begins going down pathways that are open and working freely, so there is no “traffic.”
What Causes Varicose Veins?
The simple cause is venous insufficiency. This means the veins aren’t working properly and there are a few reasons why this happens. It could be genetic. Mom or Dad had them and you simply have them because of genetics.
It could be that the patient worked on their feet for many years. In the case of extensive standing, gravity is always pulling blood down towards our feet, while our veins are trying to pull blood back up to our heart, so there’s a constant battle in that the veins are always working against gravity.
Venous insufficiency can also be worsened by pregnancy. You may have a baby in the belly that is pushing on veins and not allowing those veins to bring blood back up to the heart. The baby can cause resistance in the blood traveling from the lower legs to the heart.
How Do Varicose Veins Develop?
As veins are put under the tremendous stress of having to work against gravity, during pregnancy or after knee surgery or hip surgery, the quality of vein seals begins to decrease.
The seals in the valves inside the veins no longer make sufficient contact and they start to get stretched out which then allows blood to go backward, stretching them out even more. It basically becomes a vicious cycle.
As the vein keeps getting more and more dilated, the valves work less and less efficiently. Over time, the vein ceases function almost completely. At that point, the veins get so big that blood is basically just sitting there, pooling, not circulating back to the heart.
To combat this, the “bad traffic lane,” so to speak, needs to be avoided and the blood has to go a different route, a route that’s actually working. This way, the blood will move so much faster and more efficiently. The end goal is to get the blood to the heart and ultimately to the lungs t0 get appropriate oxygen again.
What Are the Effects of Blood Building up or Going the Opposite Way in the Body?
Initially, much swelling happens in the lower extremities as well as discoloration. Shins can become brown and hair on the legs can even stop growing. Circulation can become so poor that feet turn cold and you can develop open sores, like ulcers, which can bleed and refuse to heal. This becomes a hotbed for infection.
Additionally, patients tend to experience painful legs, heavy legs, aching, soreness, cramping, restless legs, and even trouble sleeping at night because of constant cramping and throbbing in the legs. While there are multiple reasons for restless leg syndrome, one of them is the poor circulation due to insufficient veins.
When Should a Patient Visit the Doctor About Possible Varicose Veins?
If a patient is experiencing symptoms, it’s probably already time to get the veins assessed, as many patients do not experience symptoms at the onset. Symptoms include pain, aching, soreness, cramping and swelling.
If these symptoms begin to interfere with your daily life and activities, it is time to visit the doctor. The ultrasound for diagnosis is painless and takes just 20-30 minutes to complete. It’s a quick, easy and non-invasive screening test. It is good for peace of mind to know if you’re dealing with varicose veins, at risk of a more serious condition, or even something unrelated/benign.
It also allows patients time to prepare for eventual treatment such as wearing compressions to battle insufficiency.
How Are Varicose Veins Diagnosed?
Before beginning any treatment, you should rely on information revealed in an ultrasound of the legs. This shows how blood is flowing, if there is any backflow going the wrong direction, and if the veins
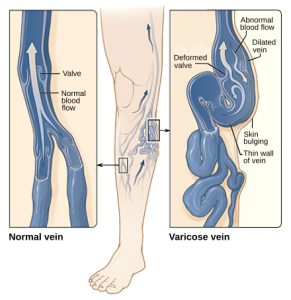
have been stretched out or dilated. Once the veins become stretched out and dilated, the little doors inside the vein that are supposed to keep blood going in only one direction no longer make a good seal, so blood goes in the wrong direction and they become leaky. Normal veins have tight valves that
don’t let the blood go in the wrong direction. In the progression of varicose veins, those valves stop working, blood starts going backward, veins begin to stretch, and other symptoms appear, like swelling and discoloration.
What Other Diagnoses Could These Symptoms Indicate Other Than Varicose Veins?
If the veins are competent, meaning the patient is not getting backflow of blood and the veins are not too stretched out, then circulation issues, such as varicose veins, are eliminated from the discussion.
It could be arthritis, a nerve pinch, or diabetes. Restless leg syndrome and other musculoskeletal or vascular issues are also in the conversation.
Does Insurance Cover the Ultrasound?
Yes. If there is reason for investigation, symptoms like pain, swelling, or aching, insurance should definitely help pay for that.
What Is the Treatment Option?
Cap treatment is most prominent. The cap, is endovenous, meaning it is an “inside the vein” laser. A little wire is inserted into the bad vein using ultrasound to help locate the treatment point exactly. The ultrasound tells us that we’re in the vein and we’re using the laser in the correct area. The cap then seals the poorly-functioning varicose vein
In terms of pain, most people are not bothered. Some local numbing is issued around the vein that is going to get lasered. A few shots of numbing make it very comfortable. The shots feel like pressure and the laser procedure itself has been described as a tugging feeling. Patients feel a little bit of pushing and pulling but there’s no sharp pain.
How Does Quickly Does the Endovenous Laser Work?
The endovenous laser is made up of a catheter that seals the vein shut immediately. After a week, the ultrasound shows over 99% of the time that that vein has been shut down and is already recirculating that blood through better working channels. Patients typically walk out on their own and many times they actually feel better within that first week. They are able to return to daily activities right away. Getting up and walking around immediately is key for getting the blood to recirculate.
that blood through better working channels. Patients typically walk out on their own and many times they actually feel better within that first week. They are able to return to daily activities right away. Getting up and walking around immediately is key for getting the blood to recirculate.
What Are the Risks if Varicose Veins Are Left Untreated?
The biggest worry is developing a venous ulcer. It can bleed and become infected, serving as an entryway for bacteria to get into the bloodstream. When the skin breaks down like that because the blood is literally not moving, worsening symptoms can result.
Another concern is blood clots causing thrombosis in the deep vein. Those can be extremely painful, but more importantly, can then become embolized which means the clot shoots off and travels up to the heart and then to the lungs, which then can cause a pulmonary embolus. This blocks blood flow to the lungs, so the patients do not oxygenate. Pulmonary embolisms are truly life-threatening.
As far as smaller issues, patients can accumulate a lot of swelling which can then make it hard to move. It can cause rashes on the skin because the skin doesn’t like it when the blood isn’t moving around and is just pooling. The patient can contract a type of dermatitis called stasis dermatitis. That is when the blood just stays down in the lower legs and doesn’t move much. As the blood is pooling there, the iron in the red blood cells can stain brown in the skin. This is coupled with an itchy rash.
Why Are Varicose Veins Most Common in the Legs?
Simply put, if veins in the legs have to work against gravity to push blood up to the heart, they can wear out and become incompetent.
Typically, a saphenous vein is affected. These are one of the main veins on either side of your legs. There is upper and lower half to it so patients can technically have up to four areas that need to be treated. The ultrasound guides the doctor in diagnosing the troubled regions. The ultrasound might say “Your left lower is working just fine. It’s your left upper that needs attention and immediate treatment.” A few years later, the lower half may require treatment, but that wasn’t the initial need. Insurance companies rely on the ultrasound to diagnose severity and essentially decide when treatment will be accepted.
If you have additional questions or are struggling with the possibility of varicose veins, contact Universal Dermatology.
Lear MoreSPIDER VEINS – DEFINITION, CAUSES AND TREATMENTS
Spider veins. We’ve all heard the complaints, especially during shorts season.
“My legs look terrible!”
“How did this happen?”
“Am I going to look like this forever?”
The good news is spider veins are not medically dangerous and are easily treatable. (more…)
Risk Factors for Varicose and Spider Veins
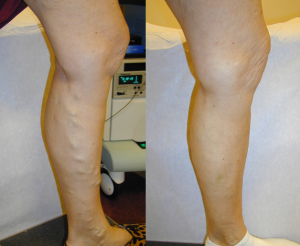
A large percentage of the US adult population experiences some type of vein disorder. In fact, it’s estimated that up to 40% of US adults experience a vein disorder. Varicose and spider veins are among the most common vein disorders. Varicose and spider veins vary in either being purely cosmetic issues or being related to a deeper venous problem. Common risk factors for Varicose veins and spider veins include:
- Heredity
- Standing often at work
- Obesity
- Hormonal changes during pregnancy, puberty, and menopause
- The use of birth control pills
- A history of blood clots
- Conditions that cause increased pressure in the abdomen including things such as constipation, tumors, and externally worn garments like girdles.
- Women are more at risk than men
If you have spider or varicose veins, or are experiencing more concerning symptoms such as leg pain, swelling, heaviness, or even restless legs, call on a Universal Vein Care expert to diagnose and treat your condition. Our clinical services encompass all elements of vascular care, including Vericose vein removal, diagnostic evaluations, minimally invasive procedures and outpatient services.
Lear More
 Our Dermatologists
Our Dermatologists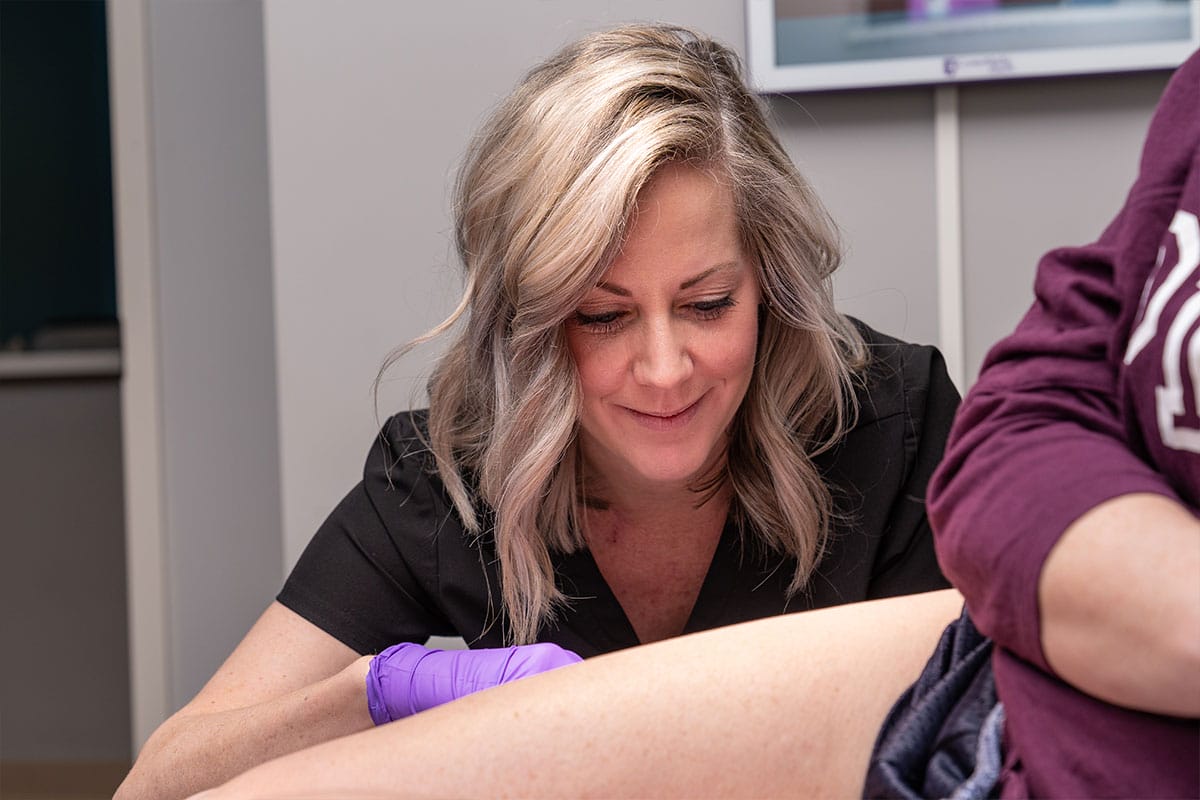 Our Providers
Our Providers Our Staff
Our Staff Specials
Specials Financing
Financing Pay Bill Online
Pay Bill Online